
I landed on time, with an announcement over the intercom of, “Welcome to Liberia. This is the last Delta flight into Monrovia. God bless you all.”
Charming, no?
That set the tone for me right away. I became sick that same night, starting with a sore throat at dinner, then a full-blown headache that turned into a migraine. If it hadn’t been for the timing, I sure as hell would have worried about Ebola. But my rational mind said it couldn’t be — I’d started to get sick too quickly, so I marched on, with three days of pure hell, between my bed, the bathroom and the Ministry of Health.
Since I’ve recovered, I’ve been staying in the south east of Liberia, working for a small but efficient Liberian-American NGO called Last Mile Health, one of the very few NGOs remaining actively present on the ground in Liberia helping the country with its Ebola response and preparedness. My focus is to provide the much needed training of healthcare workers around Ebola management, in partnership with the national and county health teams.
What you hear in the news about how bad the Ebola crisis is in Liberia is an understatement. Most of what you hear about are the deaths, the cases, fear, the epidemic concentrated in Monrovia, the capital. That is all sadly so real. But those reports ignore the other elephant in the room: God forbid, when Ebola spreads to the rest of the country, any efforts of containing it at the response rate we are seeing today will be ineffective.
And here’s why:
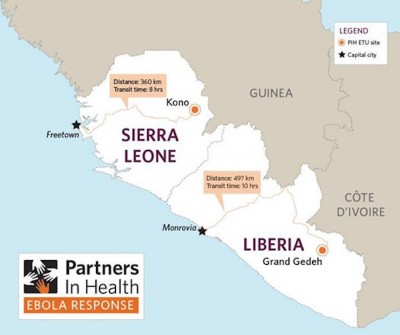
As of today, there is only one laboratory in Liberia to analyze blood samples of suspected patients, and it is in Monrovia. That means that a suspected Ebola patient that has been quarantined in the south of the country will get his results at least three days later (it’s normally a six hour test).
In the meantime, those suspected patients are clogging your isolation units, increasing their risk of getting the disease from those who actually do have it, and preventing access to isolation facilities for those who truly need to be quarantined from the rest of the population.
Why the WHO is not sending portable labs to the rest of the country is anybody’s guess.
Furthermore, all the Ebola Treatment Units (ETUs), where probable and confirmed cases are sent for treatment, are in Monrovia as well — and they are full. There are reports of sick patients coming from other counties who are turned back — but to go where?

More likely, they die on the way, as Liberia’s national “highway” is a constant crater of mud and stuck trucks and in need of massive repair. It takes a grueling 12-15hours in a 4 wheel drive to make the 300 miles to reach Monrovia from Zwedru, the capital of Grand Gedeh, in the South East of Liberia.
Most concerning however is the fact that the healthcare staff in the rest of the country remains in urgent need of training on Ebola: how to triage sick incoming patients, how to handle patients safely, how to implement strict infection control measures, how to clinically manage patients or how to provide psychosocial support.
Despite being the front line workers of this crisis, they disconcertingly still lack that education and basic equipment like personal protective clothing to be able to safely and humanely manage a potential case of Ebola. Trainings are being developed, but it is appallingly late. As of yet, no one has showed up at the clinics and hospitals to actually conduct them.
In the communities outside of Monrovia, a push for awareness and social mobilization efforts has taken place. But improvisation is really the name of the game and much remains to be done.
In the meantime, we have a national curfew, and roadblocks every few kilometers for hand washing and to check our body temperatures (I have been clinically dead at 32.3 C a few times, but that didn’t deter them to smile and tell me “all good!”)
The county of Grand Gedeh, where I am, has so far stayed relatively free of Ebola cases — and has now quarantined itself to protect the population. But how secure is this barrier really, and how long can it last?
Hundreds of Liberians have been stranded at the border for days with little food, prevented from entry into this “safe haven.” Some reportedly have managed to cross somewhere else by canoe.
There have been reports of sick people being turned around — but where should they go? Frighteningly, they become lost contacts and most likely end up infecting others, perpetuating the spread of the disease.
Liberia needs to combat an epidemic that, according to the country’s defense minister, “threatens Liberia’s national existence.” In the midst of this desperate situation I am asking, where is the help? Where are all those NGOs who rushed to assist during the Banda Aceh tsunami and other recent global crises?
The reality is that they have for the most part been conspicuously – and frankly, embarrassingly — absent from this disaster response, withdrawing their staff or choosing not to come at all under the pretense of protecting their staff.
These excuses are unacceptable and I worry that fear, not sound science and common sense, are driving their decisions.
The thing is, there is a plethora of other interventions international NGOs can provide besides working in the front lines taking care of dying Ebola patients. There is plenty of critical work to be done that doesn’t require one to be exposed to the virus — for example educating healthcare staff in sound infection prevention and control measures, social mobilization, community awareness, logistics or communication.
Last week, the Gates Foundation had made a $50 million contribution to the Ebola crisis — the largest emergency relief grant the foundation has ever made. But that’s only a sliver of the $600 million the WHO says it needs to fight the outbreak. And those dollars aren’t a substitute for the staff, clinical knowledge and experience that medical aid organizations can provide.
So please NGOs, Liberia is desperate need of help.
To help with Ebola relief in Libera, consider a donation to Partners in Health, Last Mile Health or Doctors Without Borders.

